What is Bone Marrow Transplant
Bone Marrow Transplant procedure is performed not only for cancerous conditions like blood cancer but also for a genetic condition like Thalassemia. Here, the cancerous or genetically abnormal stem cells are eradicated by chemotherapy and immuno-suppressive medicines, and new functionally normal stem cells are given, which later populate the bone marrow and blood with normal, non-cancerous, and genetically normal cells.
Enquire Now
BMT
For the FIRST time in the state of Andhra Pradesh, Mahatma Gandhi Cancer Hospital & Research Institute
Visakhapatnam, which has been in health care service for more than 19 years, is the largest comprehensive, exclusive cancer specialty hospital in Andhra Pradesh, with the largest team of qualified cancer super specialists under one roof, drawn from all premium institutes in India. We are equipped with cutting-edge technology for patient-centric oncology care with evidence-based medicine practices ranging from prevention, early detection, cancer-treatment, and terminal care.
The Mahatma Gandhi Cancer Hospital has the state of the art bone marrow transplant (BMT) unit, which is equipped with HEPA filtered and Positive pressure ventilated (PPV) transplant suites. The unit also consists of stem cell laboratory, Flowcytometry for stem cell analysis and a stem cell aphaeresis machine. We perform both allogeneic and autologous stem cell transplants. Our bone marrow transplant facility is the first of its kind in the state of Andhra Pradesh.
The stem cells in one’s healthy bone marrow are responsible for producing blood cells, especially leukocytes or white blood cells (WBCs) that are essential for the immune system. Blood cancers and their associated treatments, such as chemotherapy and radiation treatments, deplete your bone marrow. Stem cell transplants help in regenerating new cells from the old cells to help your body create more cancer-free cells. The stem cells can be collected either from your own bloodstream or from that of a donor.
Here’s how the transplant process looks
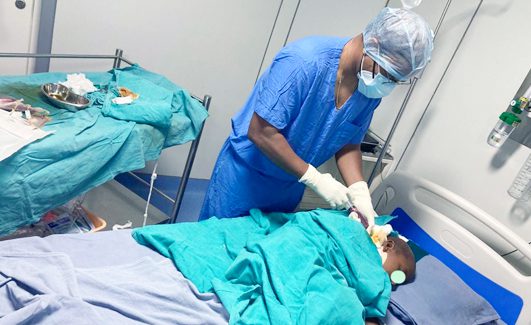
Before the transplant
- Before the blood is drawn out, you or your donor will be injected with medicines to transfer blood-forming stem cells from your bone marrow to your bloodstream.
- The stem cells from you or your donor’s blood will be collected, separated from the bloodstream, and kept in a frozen state.
- You go through a conditioning treatment which involves high or low doses of chemotherapy or radiation to kill the cancer cells and your own stem cells so as to replace them with new stem cells.
During the transplant
- The infusion procedure begins with you sitting in a chair and the infusion passing through a venous line attached to your neck.
- You will be monitored for any fall in temperature or blood pressure or the development of a fever.
- You may experience some side effects, such as headache, nausea, and shortness of breath.
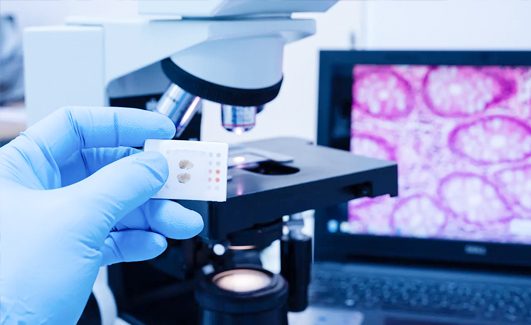
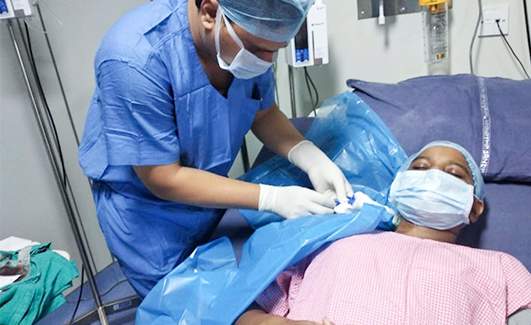
After the transplant
- After the transplant is complete, the infused stem cells will start grafting into the bone marrow over a period of two to four weeks. Next, they will also start producing white blood cells, platelets, and red blood cells.
- In case the stem cells are from a donor (Allogeneic Transplant), you will need to take antibiotics and anti-rejection medicines to help your body accept the transfused cells. You may also need transfused red blood cells, platelets, and nutrition.
- You may need to stay in a hospital for a month until your immune system starts functioning. It’s important to stay in a germ-free environment.
- You will need to visit the outpatient section so that the doctors can check your blood and bone marrow for any complications.
Mahatma Gandhi Cancer Hospital & Research Institute has launched its state-of-the-art Bone Marrow Transplant (BMT) facility at HealthCity, Arilova, Visakhapatnam, which is the first such exclusive BMT unit in Andhra Pradesh. The unit has four transplant cubicles for transplant patients’ use before and after the procedure. All cubicles are of class-10000 clean room standard and equipped with HEPA filtration systems and positive pressure ventilation. The transplant program team provides a specialized service under the Hemato Oncology department. The team is committed to providing quality service to all children and adults needing this procedure.
About Bone Marrow
Bone Marrow is the soft and spongy tissue found within bones which is rich in stem cells. The most primitive of these stem cells are the pluripotent stem cells, which are different from the other cells in the following aspects :
- They produce cells identical to themselves
- They have the capacity to produce one or more subsets of mature cells
These stem cells are of prime importance in Bone Marrow Transplant, which is more appropriately known in clinical terminology as Hematopoietic Stem Cell Transplant (HSCT).
Other sources of stem cells have gained popularity in the last decade, because their harvesting is better tolerated by the donor and delivers almost identical success rates when compared to Bone Marrow Transplant. These include Peripheral Blood Stem Cells and Cord Blood Stem Cells.
Some Conditions which require Bone Marrow Transplant ( BMT)
The conditions which necessitate a Bone Marrow Transplant (BMT) can be broadly classified into 2 groups
Cancerous Conditions
- Acute Myeloid and Lymphoblastic Leukemia
- Chronic Myeloid and Lymphocytic Leukemia
- Relapsed Hodgkin’s and Non-Hodgkin’s Lymphoma
- Myelodysplastic Syndrome
- Myeloproliferative Neoplasms (Primary Myelofibrosis, etc)
- Multiple Myeloma
Non-Cancerous Conditions
- Aplastic Anemia
- Haemoglobinopathies such as Thalassemia and Sickle Cell Anemia
- Immunodeficiencies disorders
- Inborn errors of metabolism
- Storage disorders
The procedure of Stem Cell Transplant
Before a stem cell transplant, stem cells are collected from either the bone marrow or the blood. The patient is given high doses of chemotherapy, usually over a few days. Sometimes, radiotherapy is also given to the whole body, known as total body irradiation (TBI). This process is known as “conditioning”.
As well as destroying any remaining cancer cells, the high doses of chemotherapy also destroy the stem cells in the bone marrow. After the chemotherapy, the patient is given the stem cells that were collected before the treatment. These stem cells start producing mature blood cells again.
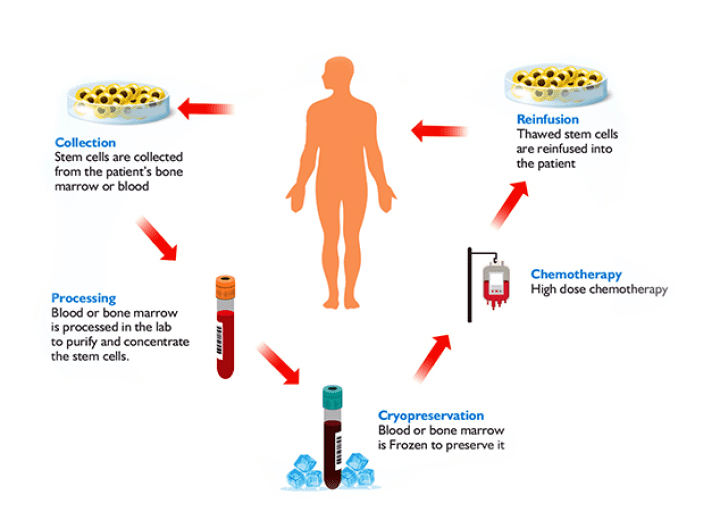
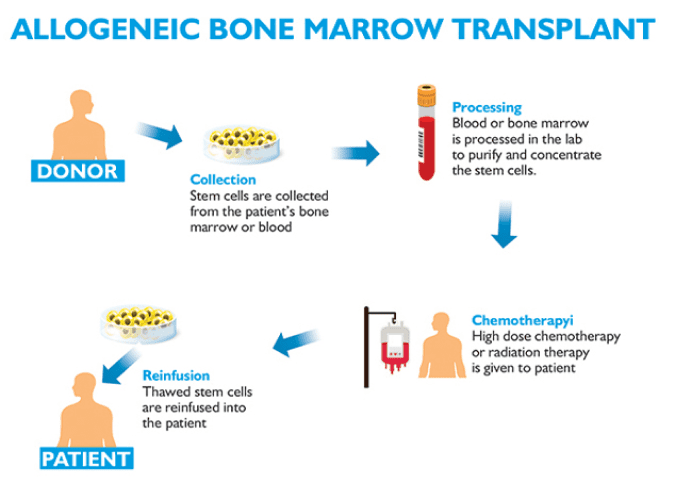
_ Types of transplant _
There are Two main types
A. Autologous BMT
In this procedure, patients own stem cells are collected and these stem cells are used after the high- dose treatment.
B. Allogeneic BMT
This uses stem cells from a donor and also known as an allograft. An allogenic transplant is more complicated procedure than an autologous one and only carried out in a very few specialized hospitals in India. Recovery may take several months or longer. The donor is another person whose tissue has the same genetic type (HLA type) as the person needing the transplant (recipient). It is more likely that the recipient will find a suitable donor in a brother or sister. This however, happens only 25 to 30 percent of the time.
If a family member does not match the recipient, the request is sent to the unrelated bone marrow transplant registry database to look for a suitable unrelated individual whose tissue type is a close match. It is more likely that a donor who comes from the same racial or ethnic group as the recipient will have the same HLA type.
Steps involved in Bone Marrow Transplant
Peripheral Blood Stem Cell Collection
The Peripheral Blood Stem Cell Transplant Method is more commonly performed when compared to the Bone Marrow Harvest Method, and it is less invasive and easier to perform. Some studies even suggest that the stem cell yield by this method is higher when compared to bone marrow harvest. The process takes 4-6 hours after administering the necessary medication for 4 days.
Conditioning of the Patient
- The conditioning process involves high doses of chemotherapy and sometimes radiation. It is carried out for three reasons :
- Destruction of the existing bone marrow cells to make room for the transplanted stem cells
- Destroy any existing cancer cells
- Suppression of activity of the immune system to decrease chances of rejection of donor stem cells.
Transplanting the Stem Cells
The process of Bone Marrow Transplant does not involve the physical insertion of the marrow stem cells into the marrow of the recipient. It is more of an intricate and delicate blood transfusion method. The harvested stem cells are administered via a central venous catheter into the bloodstream. The donor stem cells have the property of stem cell homing, whereby they migrate to the patient’s bone marrow and override his defective stem cells. This restores the ability of the patient’s bone marrow to produce blood elements.
Risks of Bone Marrow Transplant (BMT)
1. Graft versus Host Disease (GvHD)
In this disease, the transplanted stem cells (“graft”) attack the recipient’s cells (“host”) as they are recognized as alien cells.
There are two types of GvHD
Acute GvHD – Occurs during the first three months following the transplant.
Chronic GvHD – Develops after 3 months and can cause symptoms for many years.
Chronic GvHD – Develops after 3 months and can cause symptoms for many years.
2. Infections
As a consequence of chemotherapy and bone marrow suppression, the body is transiently unable to procedure cells to combat infections.