
Enquire Now
Adaptive Radiotherapy
Adaptive Radiotherapy is a treatment technique that can systematically improve its treatment plan in response to patient/organ temporal variations observed during the therapy process.
Variations in patient/organ shape and position could occur during the radiotherapy course. Consequently, the radiation dose delivered to the target and critical normal organs can significantly deviate from planned doses. It is important that we identify these changes happening during treatment and modify the plan using ‘Adaptive Radiotherapy’ so as to deliver accurate doses to the tumor while reducing normal tissue toxicity. Optimized target coverage and normal tissue dose with adaptive replanning based on tumor response.
Radiation therapy has evolved over the past two decades and its precision and accuracy has improved incredibly. This was possible with the introduction of various imaging techniques like contrast CT scan, multi-parametric MRI and PET CT scans, along with computerized radiotherapy planning techniques like IMRT (Intensity Modulated Radiation Therapy), VMAT (Volume Modulated Arc Therapy) and IGRT (Image Guidance Radiation Therapy) with onboard imaging technique like CBCT (Cone Beam CT scan) which is an in-built CT scan in the Linear Accelerator.
With the above-mentioned techniques, we could only assess the position of the patient and the dose contributing to the normal structures in that particular treatment session. However, radiation therapy is usually delivered over a six to seven weeks period and we know that the tumor and the patient change in shape over this period. This dynamic change in the position of the tumor and organs at risk (OAR) is due to various factors like movement with respiration, differential filling of rectum and bladder, change in the shape of tumor (either shrinkage or progression), and weight loss of the patient. All these factors can decrease the precision of the radiation therapy and the cumulative dose delivered to a particular organ or the tumor cannot be accurately estimated, which may decrease the therapeutic ratio.
With advancements in IGRT, we can identify anatomical changes at the earliest and do replanning on newly acquired planning CT scan. However, this process does not allow us to gain knowledge about the delivered dose, toxicity rates and benefits of adaptation.
Adaptive radiotherapy (ART) is a radiation process which addresses patient-specific treatment variations, including systematic changes in weight loss, tumor and organ geometry and biological response as well as stochastic variations such as organ deformation, filling change and respiration or peristaltic movements.
To address the above issue, Raysearch enables us with sophisticated ART technology like Deformable Image Registration (DIR), dose deformation and dose accumulation. With the help of Deformable Image Registration (DIR), it is possible to do auto-segmentation (i.e. delineation of target and normal structures) on the CBCT and allows assessment of daily dose. Further sophistication, it allows for the accumulation of dose in the tumor and OARs over the course of treatment. This empowers the radiation oncologist to make a decision on ART (replanning and treatment delivery) based on accumulated doses rather than independent snapshots.
Adaptive radiation therapy can be binned into three major classes:
- a) Offline – this is done between fractions to address systematic and progressive changes during treatment. It is mostly done in head and neck, lung and prostate.
- b) Online – This is done immediately prior to treatment fraction. It is done particularly in abdomen and pelvis where offline ART is insufficient to account to variations
- c) Real time – which is done during the treatment of fraction. Example – MRI guided ART in prostate cancer.
The main steps of ART are –
1) Image acquisition – ART needs adequate information of tumor, OAR delineation, and accurate dose calculation which is possible with sufficient image quality of CBCT (iterative).
2) Deformable Image Registration (DIR) – This is an important step in ART to account for changes in the shape and size of internal organs between initial and adaptive planning images. The images are usually acquired at every fraction prior to treatment delivery to perform tasks such as deforming contours and electron density mapping. It helps in contour propagation, plan adjustment and fractional dose accumulation. There are various qualitative and quantitative measures for evaluating the image registration accuracy to reduce errors.
3) Dose accumulation and tracking– As the anatomy and corresponding contours change, the initial dose calculated using the planning data set may have limited accuracy and may not represent the actual dose delivered. ART provides summary of delivered dose, by voxel by voxel dose accumulation for each delivery time point. This “dose of the day “ is warped back to initial planning CT scan for dose accumulation over the total fractions to date. The methodology of deforming adaptive planning image yields improved dose estimation.
4) Rapid Replanning – Replanning cases for ART involves consideration of stratgegy ( online vs offline), delineation of targets and OARs, time taken for replanning and clinical criteria for adaptation.
5) Pre treatment planning and delivery quality assurance – Offline ART strategies follow standard treatment plan and delivery QA approaches that EBRT planning workflow. Online ART needs automated plan check and secondary dose calculation tools for independent evaluation of plan quality.
Raysearch even helps with artificial intelligence (AI) in various components of ART, like auto-contouring and autosegmentation, registration, planning and quality assurance. Raysearch is enabled with model based and atlas based segmentation which has the capability of machine learning.
We at Mahatma Gandhi Cancer Hospital & Research Centre are mainly focusing on lung, head and neck, prostate and cervical cancers to improve therapeutic ratio with Adaptive Radiotherapy.
Fig 1 : Flowchart showing increased levels of adaptive radiotherapy, ranging from simple IGRT based replanning to DIR based dose accumulation and development of predictive models tied to an outcome database
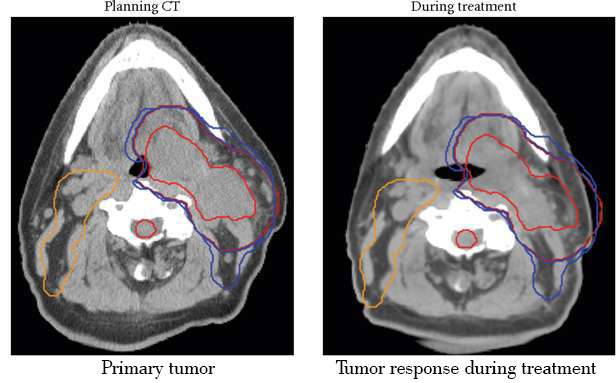
A&D – represent the primary nasopharyngeal tumor and neck nodes prior to starting RT. B&D represents shrinkage of primary and nodes after 12 fractions. C& F represents deformation of image to propagate the contours and dose for adaptive plan.








